Pathologists’ Role in Precision Oncology Care
My experience delivering diagnostic pathology services within the laboratory and in the patient exam room have made clear the importance of pathologists serving alongside oncology care teams. The success of these collaborations is driving change in the pathologist’s role in providing precision care.
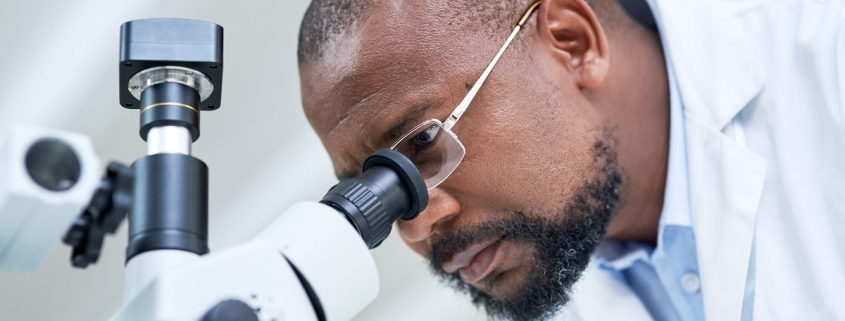
A complete and accurate pathology report is crucial to diagnosing patients and deciding on the best treatment plan. Pathologists are highly skilled and experienced members of the care team, specializing in interpreting laboratory tests and evaluating cells, tissues, and organs to diagnose disease. We use state-of-the-art equipment and the most advanced techniques to analyze tissue samples.
As part of my journey, I’ve participated in diagnosing multiple challenging and interesting cases and have collaborated with our network’s oncologists by providing crucial laboratory results that determine an array of cancer therapeutic decisions.
Pathology Reports Are Not Always Clear
Pathologists’ important work on the oncology care team can often be obscured by reports that are not meant for patient consumption. In particular, pathology and ancillary test reports are not written at a level most patients can understand. It can be discouraging for the diligent and engaged patient who proactively seeks out detailed information about their lab results and what these might mean for the prognosis.
According to the Association of Community Cancer Centers, these reports may also be organized in ways that are confusing to both clinicians and patients. While some patients may meet or speak with pathologists, most pathologists don’t have the time or training to explain their findings directly to patients – a significant hurdle in today’s healthcare environment.
However, as calls for advancements in precision medicine grow louder, so too are calls for ensuring information from pathology is presented in a consumable, patient-friendly manner. The National Academy of Medicine recommends “good communication about key findings” of the reports for patient use. “Pathology report and ancillary test results are integral to patients fully understanding their disease, treatment options, and participation in shared decision-making. Put another way, when patients can access the key information from their pathology and ancillary test reports, in patient-accessible formats, patients can be empowered to understand their disease and treatment options better and engage in the shared decision-making process with their care team.”
Delivering Consumable Pathology Reports for Patients
To deliver the highest level of consumable information about the precise nature of a patient’s condition, some steps to take may include giving the patient a list of reliable sources for additional information about their cancer, connecting patients to cancer-specific advocacy and support groups, and providing patients with patient-centered education and resources for additional information, such as clinical trials.
Clinicians have access to experts and resources designed to help them better understand the information contained in pathology and ancillary test reports. Paired with the reports prepared by pathologists, which they can use to guide shared decision-making conversations about treatment plans, patients can use this information to refresh their memory about the details of their condition before speaking with clinicians.
The role of pathologists is increasingly vital in the practice of precision cancer medicine because of the continuous advances in genomic and molecular testing and the transformation of the traditional exclusively high-level practice of pathology into a more molecular-based medical specialty, as well as the desire for more consumable information related to precision medicine.
Continuously adapting with the newest medical discoveries to provide the most accurate and informative cancer diagnoses for our patients remains paramount, but it’s only one of our charges. By integrating pathologists into patient care teams, we can provide more comprehensive strategies for managing information sharing and meeting the requirements of precision medicine for all patients in our network.
Engaging patients in portions of their care, even those areas that can be difficult to translate and communicate, is a step toward holistic, whole-person care.